Writer’s Note:
I’d like to take a minute to explain the delay in publishing this final post of our serial newsletter Are People Losing Their Minds? I was on track to complete the post in a timely manner when I encountered the latest variant of Covid-19.
Despite being immunized 3 times, Covid prevailed.
I appreciate your understanding and hope you haven’t lost interest and confidence in our work.
Part 1 of the newsletter posed this question: are increasing incidents of spontaneous and public interpersonal violence a signal that our social fabric is unravelling?
Part 2 explored possible reasons for this rise in anti-social behaviors. In particular, the function of two important areas of the brain - the amygdala and the prefontal cortex - and the vital role each of them play in regulating emotions and the consequences when one or both don’t work as designed.
Part 3 - this post - explores the root causes of emotional dysregulation as documented in research studies; and how that knowledge might be helpful in understanding what’s fueling the current anti-social behaviors.
There is also a discussion of how strategies and techniques used to treat mental health disorders that feature emotion dysregulation might also be effective in addressing the rise in hyper-reactive and violent incidents that are now regularly featured in the news.
Before we dig in, it’s important to note that these posts do not suggest there is any equivalency between mental health conditions that feature emotional dysregulation traits, such as BPD, ADHD, PTSD, anxiety, depression and others, and the random, angry and violent attacks perpetrated against strangers that fill the news cycles.
Rather, the message here there may be opportunities to identify a therapeutic strategy that’s been effective in treating of people with mental health disorders may be helpful in addressing the broader issue of untreated individuals who experience out-of-control emotional dysregulation that causes harm to others.
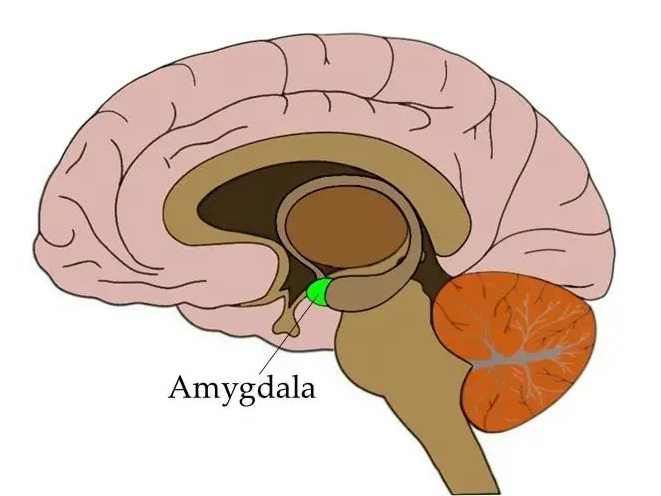
Many of the processes involved in emotion regulation take place in two specific areas of the brain: the amygdala and the pre-frontal cortex, or PFC.
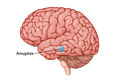
The amygdala is an almond-sized structure located in a lower part of the brain known as the limbic system. Made up mainly of specialized nerve cells or neurons, the primary emotion the amygdala processes is fear.
The pre-frontal cortex is located in the front of the skull just behind the eyes. The PFC is where the so called executive functions, such as reasoning, planning, decision making and impulse control, are formed and implemented.
When the amygdala detects a potential danger in the outside environment, the neurons that make up the amygdala relay that information to the pre-frontal cortex for a deeper assessment and response to the danger, e.g., the fight or flight reaction.
Sometimes, however, that amygdala/PFC loop becomes overwhelmed and the emotional regulation process gets disrupted and rendered dysfunctional.
As noted, there are many people diagnosed with mental health conditions that experience emotional dysregulation. But brain imaging studies have also documented similar physical and functional alterations to the amygdala and pre-frontal cortex in people who experience ‘hair trigger’ bouts of anger that often provokes aggressive and violent behaviors.
One thing: Stress.
Over the last 4 years, people’s lives have been deeply altered by the impact of the highly lethal Covid-19 pandemic. The catastrophic global health crisis caused 7 million deaths and led to enforced social isolation; forcing a majority of people to work from home; and children to learn while sitting alone interacting with a computer screen, absent their social circle of friends.
There were also controversial mandatory masks rules for public places like stores. Other activities outside the house such as dining, going to movies, concerts, lectures, sporting events and other public gatherings were ground to a halt.
Adding to the stress caused by Covid-19 are the disastrous effects of climate change: massive wildfires, melting icebergs, deadly earthquakes, record floods, tornados and hurricanes.
As if that were not enough, people lives have been further stressed by a toxic mix of social media technology and divisive social and political discord.
As noted, the roots of the Amygdala / Prefrontal Cortex disruption are directly related to the increasingly higher levels of stress that had come into our lives.
And the impact of unrelieved stress on the amygdala and PFC is significant.
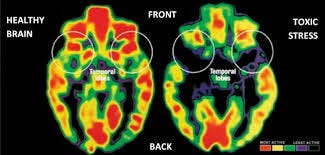
A 2010 study published by the journal Social Cognitive and Affective Neuroscience, concluded that the impact of stress on the amygdala and the Pre-Frontal Cortex can not only alter their physical structures, but disrupt the way they functions a well.
“Even quite mild acute uncontrollable stress can cause a rapid and dramatic loss of prefrontal cognitive abilities, and more prolonged stress exposure causes architectural changes in prefrontal dendrites.”
Other studies have shown that increased stress stimulates the amygdala to generate more neurons (nerve cells) to accommodate the increased frequency and strength of the warning signals it sends to the PFC.
But that comes at a price.
When emotions run high, blood and oxygen flow to the enlarged amygdala, and away from the diminished prefrontal cortex. This loss of cells in the PFC reduces the ability to think and solve problems effectively.
This known as ‘amygdala hijacking' - a state where when the amygdala is over active and the prefrontal cortex less active. As a result, the brain’s responses switch from the slow, thoughtful PFC emotional regulation to the more rapid and highly reactive emotional responses of the amygdala.
The point is that structural changes to both of these areas of the brain render people less able to regulate their emotions, more likely to be highly reactive, aggressive, angry and less able to control their responses.
Think about that for a moment. Constant exposure to unrelenting stress is literally damaging people’s brains and affecting their behaviors in seriously negative ways.
This begs the question:
The answer is yes. But it won’t be an easy goal to achieve.
Fortunately, there are a number readily available resources, techniques and strategies that might be helpful, notably:
Dialectical Behavior Therapy
Dialectical Behavior Therapy is a highly effective therapy developed by Marsha Linehan PhD. DBT has become the gold standard for the treatment of Borderline Personality Disorder. The social skills Dr. Linehan included in DBT are a critical part of the success of the treatment; particularly in managing out-of-control emotional responses. This includes:
Learning to recognize the emotions you are feeling
Realizing when you are starting to feel angry
Identifying what triggered the anger, and
Taking appropriate steps to calm down, using one or more of the DBT skills such as problem solving.
Prior to the 1993 publication of psychotherapist Marsha Linehan’s groundbreaking book, Cognitive-Behavior Treatment of Borderline Personality Disorder there were very few books written about BPD and emotional dysregulation.
The publication of Dr. Linehan’s book lit a bonfire of interest in BPD, particularly among young researchers. Before her book, there were very few others written on the subject of BPD.
In the years since Linehan’s book debuted, a number of consumer oriented books about DBT have become available that individuals can access to learn about and/or implement the social skills component of DBT. For example:
Author Dr. Gillian Galen, PsyD., is a child and adolescent psychologist at Harvard Medical School’s McLean Hospital. Co-author Blaise Aguirre, MD., is medical director of a program at McLean for emotionally dysregulated young people. Both are experts in dialectical behavior therapy.
I conducted a two part ZOOM interview with Drs. Galen and Aguirre that appeared in two previous Substack newsletters.
Part One can be found here. And Part Two here.
In addition to learning and practicing DBT skills, there are several other recommended activities an individual can incorporate into daily life. They are easy to learn, but require some commitment - and practice - to be effective.
Mindfulness is a foundational social skill taught in Dialectical Behavior Therapy.
Mindfulness is a conscious effort to focus on what is happening in the present moment, not dwelling on the past - which can’t be changed; nor worrying about the future- which cannot be known. The point is that the only thing that one can control is the present.
According to the online professional educational organization The Science Of Psychotherapy: “Practicing mindfulness can enhance prefrontal activation, which is correlated with increased well-being and reduced anxiety.”
In another article, the American Psychological Association found that, “Mindfulness training holds promise for treating mood disorders partly because it appears to lead to changes in patients' brains, improving connectivity among some brain areas and changing tissue density in key regions.”
A research study published in the journal Social Cognitive and Affective Neuroscience - Stress Reduction Correlates with Structural Changes in the Amygdala- stated that:
“We conducted a longitudinal (long term) MRI study to investigate the relationship between changes in perceived stress with changes in amygdala gray matter density following a stress-reduction intervention (mindfulness meditation). To assess whether the amount of individual meditation predicted the improvement in stress, the number of minutes of meditation that participants reported on daily logs was correlated with the magnitude of their reduction in stress.”
Practicing Gratitude
Sociologist Georg Simmel called gratitude “the moral memory of mankind.” This is how gratitude may have evolved: by strengthening bonds between members of the same species who mutually helped each other out.
To investigate how gratitude impacts bonding and empathy, pioneering research has been exploring what gratitude actually looks like in the brain.
These and other studies found that grateful brains showed enhanced activity in two primary regions: the anterior cingulate cortex (ACC) and the medial prefrontal cortex (mPFC). In addition to emotional regulation, these areas have also been associated with interpersonal bonding, rewarding social interactions, moral judgment, and the ability to understand the mental states of others.
Helping others
A recent report in the online journal Plos examined the benefits of pro-social behavior during the Covid-19 pandemic. The authors of the report postulated that:
“Doing good feels good. In the last several decades, this simple maxim has been placed under scientific scrutiny and accumulated a sizable body of evidence that attests to its veracity. Prosocial effects have been observed among children as well as adults and in samples across the world. Aknin et al. speculate the “warm glow” of giving might be a universal component of human psychology.”
The US Centers for Disease Control and Prevention issued a list of recommendations for reducing the amount of stress in your life. These include:
Take care of your body– Try to eat healthy well-balanced meals, exercise regularly, and get plenty of sleep. Avoid alcohol, tobacco, and other drugs.
Connect with others– Share your concerns and how you are feeling with a friend or family member. Maintain healthy relationships, and build a strong support system.
Take breaks– Make time to unwind and remind yourself that strong feelings will fade. Try taking in deep breaths. Try to do activities you usually enjoy.
Stay informed– When you feel that you are missing information, you may become more stressed or nervous. Watch, listen to, or read the news for updates from officials. Be aware that there may be rumors during a crisis, especially on social media.
Avoid too much exposure to news– Take breaks from watching, reading, or listening to news stories. It can be upsetting to hear about the crisis and see images repeatedly.
Seek help when needed– If distress impacts activities of your daily life for several days or weeks, talk to a clergy member, counselor, or doctor, or contact the SAMHSA helpline at 1-800-985-5990.
The Mayo Clinic has also produced an online flyer that suggests simple everyday activities that can help reduce stress in your life:
If you find you need more help than these suggestions techniques might provide, consider calling the national 988 Suicide and Crisis Hotline or consult a crisis line directory for a help line near you
Additional Support Resources
BPDVideo.com, our BPD dedicated website provides many DBT related resources and support programs for individuals, family members, mental health providers and academic teachers. These resources include videos, books, BPD organizations, support groups and expert commentary. There is also information about and access to our 5 part, NIMH-funded video series If Only We Had Known: A Guide To BPD.
When I first came up with the idea that became this multi-part treatise on the biological and behavioral similarities between severe mental disorders such as BPD, and the abhorrent social behavior that seems to be on the rise in our society, I knew one things for sure. Any reasonable solution to the problem would be difficult to find.
In looking where this piece ultimately landed, the parts about the personal benefits of being kind to others is a pretty good definition of an altruist: i.e., someone with an “unselfish regard for the welfare of others”.
I then searched for “the opposite of altruist” and saw another wise quote in a blog posted by the online therapy network, Thriveworks.com.
“The opposite of altruists is narcissists, defined as “self-centered individuals who think and act as though the world revolves around them. They're often hard to deal with, but altruists—selfless individuals—might be the best people to take on this tough job.”
Could not have said it better myself.
I hope that some of the ideas contained in this post - being mindful, kind, grateful and caring, might be helpful to the cause.